Business Groups Try to Ax Fines for Mental Health Coverage Flaws
- Democrats eye new fines to enforce mental health parity rules
- Employer groups say move won’t solve access problems
Bloomberg Government subscribers get the stories like this first. Act now and gain unlimited access to everything you need to know. Learn more.
Democrats want to beef up enforcement of rules meant to make it easier to access mental health services using insurance. Business groups say the move won’t work and is a ploy to pay for Democrats’ wide-reaching social spending agenda.
Tucked into a once-$3.5 trillion domestic spending package is a provision empowering the government to fine health plans and employers that violate federal laws requiring access to mental health care that’s on par with other medical care. Health plans now get cited for violating the law and agree to come into compliance and reimburse beneficiaries.
Supporters of the new fines say they’ll give the Labor Department an effective tool to expand mental health coverage. Parity between mental health and other health services has been lacking for decades, often leaving people without adequate coverage for the help they need.
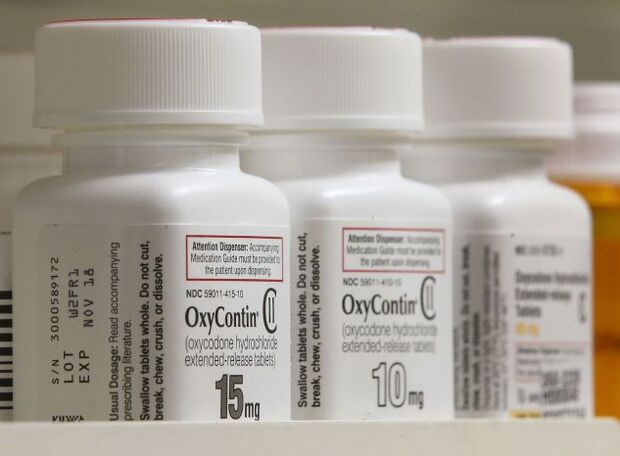
Lawmakers on both sides of the aisle say improving mental health parity in insurance plans is a key to tackling the ongoing opioid overdose crisis in the U.S. Americans are struggling to find mental health and substance use treatment services they can afford since so many services are out of network.
Employers on Hook for Mental Health Parity Despite New Target
“A crucial part of this mission is ensuring that our mental health and substance use disorder parity laws are being enforced,” Rep. Brian Fitzpatrick (R-Pa.) said recently.
“The law has to be enforced for people to start seeing a difference,” said David Lloyd, a senior policy adviser for the Kennedy Forum, an advocacy group that has led the push for the provision.
Business Pushback
Employer groups say the new fines amount to an ineffective pay-for meant to offset some of the cost of the larger spending package, which encompasses much of President Joe Biden’s economic agenda. The fines won’t address deep-rooted problems that keep Americans from accessing mental health services, such as plans’ difficulty recruiting mental health practitioners into their networks.
The new fines would bring revenue to the government, but congressional scorekeepers haven’t provided lawmakers with a final estimate of how much, according to a House Democratic aide familiar with the discussions.
Business groups say Democrats should pull the provision out of the broader social spending package.
“This won’t make a major difference in anyone’s life,” said James Gelfand, executive vice president of public affairs for the ERISA Industry Committee, or ERIC, which represents employers that sponsor health plans.
Gelfand said insurers are contending with a shortage of mental health providers in many places and doctors are reluctant to join their networks because they can get paid more charging as out-of-network providers or accepting cash. Fines won’t change that, he said.
Democrats are debating how to shrink their domestic policy package to win the support of key moderates in their party. Speaker Nancy Pelosi (D-Calif.) said Tuesday some policies may fall by the wayside to get agreement.
Democrats Divided Over How to Best Slice Biden’s Economic Agenda
Parity Struggles
Behavioral health services are far more likely to be billed out of network by providers than physical health services, which generally means higher copayments for patients, according to a 2019 report by the health consulting firm Milliman Inc. Behavioral health providers also generally see lower reimbursement rates compared to other kinds of health-care providers, the report said.
Between 2013 and 2017, the problems only worsened. In 2013, insured people were three times more likely to access out-of-network behavioral outpatient facilities relative to similar medical facilities. Five years later, behavioral care was 5.7 times more likely to be out of network.
Americans seeking mental health services often must wait to get care too, Christine Moutier, chief medical officer for the American Foundation for Suicide Prevention told the House Education and Labor Committee earlier this year.
“For those who do seek care, there’s often a long delay between the onset of symptoms and the healthcare they receive — in many cases months to years,” she said.
Federal mental health parity laws should prohibit this kind of disparity, but it’s a tall order for a small agency within the Department of Labor to enforce.
The department’s Employee Benefits Security Administration cited about 345 violations of federal mental health parity laws between 2011 and 2019. It investigated and closed 180 health plan investigations in 2020, and 3,938 investigations since 2011.
UnitedHealthcare Inks Settlement Over Mental Health Coverage
The EBSA has about 400 investigators and 100 benefits advisers to oversee more than 5 million health, pension, and other employee benefit plans, according to agency records. This means the agency has one investigator for about every 12,500 plans.
Enforcement Power
“The parity laws aren’t worth the paper they’re written on if we can’t enforce them,” said Patrick Kennedy, who founded the Kennedy Forum and formerly was a congressman representing Rhode Island.
Giving the agency the power to levy fines would create a deterrent and push health plans to better comply, said the House Democratic aide, who worked on the provision.
Mental Health Insurance Parity Gets Aggressive Focus Under Biden
Gelfand said the Labor Department’s enforcement system is working. Insurance plans often simply don’t know they aren’t in compliance or are struggling to get providers to agree to join their networks.
Instead of fines, ERIC and other employer groups are asking lawmakers to demand more from health-care providers, such as requiring them to let health plans know if they’re enrolled in any networks or participate in any telehealth programs. They’re also asking the DOL to issue more guidance around how they should comply with parity laws.
Gelfand said these solutions are harder to implement because they make demands of doctors, but they’ll improve access to care more than fines.
“Insurance companies are unpopular and beating up on them is popular,” Gelfand said. “There are tougher ways to solve this problem that involve pushing back on other constituencies.”
To contact the reporter on this story: Alex Ruoff in Washington at aruoff@bgov.com
To contact the editors responsible for this story: Fawn Johnson at fjohnson@bloombergindustry.com; Sarah Babbage at sbabbage@bgov.com
Stay informed with more news like this – from the largest team of reporters on Capitol Hill – subscribe to Bloomberg Government today. Learn more.